Autistic meltdowns and panic attacks are often treated as fundamentally different experiences. Clinically, they are. But experientially, inside the body, they can feel strikingly similar. This tension is where many autistic people are misunderstood.
The problem is not that we lack definitions. The problem is that definitions often prioritize cause and treatment while minimizing lived experience. When that happens, autistic distress gets mischaracterized, minimized, or mishandled.
Both things can be true at once:
Understanding why requires looking at what happens inside the nervous system, not just how episodes are categorized.
From the inside, both panic attacks and meltdowns involve a nervous system in alarm mode.
Common sensations include:
At this level, the body is not distinguishing why the alarm is happening. It only knows that it is overwhelmed.
This is why many autistic adults describe meltdowns using panic language:
“It feels like a panic attack.”
“My body is freaking out.”
“I can’t think or talk—I just need it to stop.”
They are not being metaphorical. They are describing high autonomic arousal.
The difference between a panic attack and a meltdown lies in how the alarm is triggered, not in how it feels once activated.
Once the nervous system realizes there is no actual danger, the surge of adrenaline and other chemicals resolves. Panic attacks are intense, but they are self-limiting.
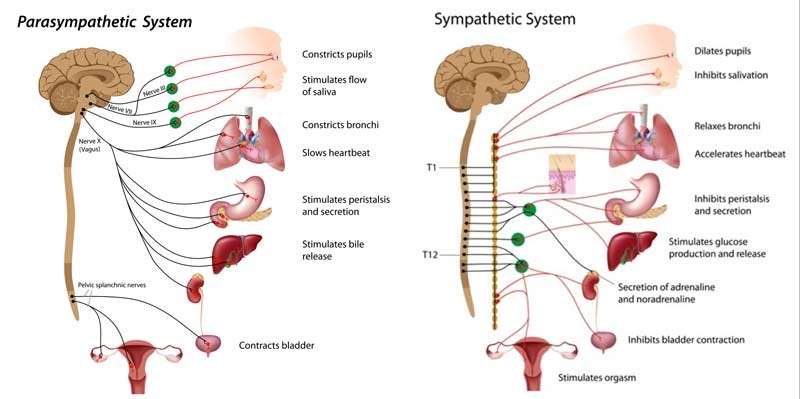
Rather than fear escalating the sympathetic portion of the nervous system, the beginning of a meltdown erodes the capacity of the parasympathetic system–the part that helps bring a panic attack to an end. Eventually, regulation by the parasympathetic system fails because it cannot process any more input.
Once the alarm state is reached, however, the body experience can be indistinguishable from panic.
For many autistic people, meltdowns feel worse than panic attacks—not because they are more dramatic, but because they involve additional layers of loss as well as the capacity of the parasympathetic system to self-regulate.
During a meltdown:
This creates a subjective experience often described as:
“A panic attack, plus sensory discomfort, plus no ability to explain what’s happening.”
Importantly, panic-style interventions like reasoning and reassurance (e.g., talking, coaching breathing, asking questions) can prolong and intensify meltdowns by adding demand when the system needs subtraction.
Panic resolves when chemistry settles the sympathetic system. Meltdowns resolve when capacity of the parasympathetic system is restored.
That difference in recovery is why we must distinguish the two, even while validating that they can feel the same in the moment.
The most useful framing is not either/or, but both/and:
Autistic meltdowns are not panic attacks in cause or treatment, but they are often panic-like in lived experience.
This formulation:
It explains why autistic people are not “overreacting,” “being dramatic,” or “mislabeling anxiety.” They are describing what their nervous system is doing.
When meltdowns are treated as panic attacks:
When panic attacks are treated as meltdowns:
Getting it right is not academic. This is a matter of safety, dignity, and recovery.
Autistic people are often told their experiences are “not anxiety” in ways that strip meaning from what they feel. A more accurate message is this:Your experience makes sense. Your nervous system is not broken. And understanding why something feels the way it does is the first step toward responding to it well.
"*" indicates required fields