The phrase “complex needs” has re‑entered autism discourse with renewed urgency, not only in clinical conversations, but across national debates about education, mental health, and disability policy.
In the United Kingdom, recent reform efforts increasingly use this language to determine who qualifies for the most intensive forms of support. As governments face rising demand and costs, “complex needs” has become a policy hinge that is shaping thresholds for entitlement, placement, and long‑term planning.
While this terminology is especially visible in the UK, similar dynamics exist in the United States, expressed through different phrases. UK systems speak more explicitly of “complex” or “most severe” needs. In the US, complexity is embedded in functional categories like “high support needs,” “medically complex,” or “behaviorally intensive.” These distinctions appear in funding mechanisms, waiver eligibility, and educational placement.
Different words, same function: whether labeled complex or high support, these terms determine who gains access to help and who does not. That makes it vital to ask where complexity truly comes from.

The phrase “complex needs” is often used as though it were self‑explanatory, implying severity rooted within the individual. In reality, complexity rarely has a single source. It emerges from the interaction of three domains: intrinsic, interactional, and system complexity.
Some autistic people experience neurological or developmental differences that create higher baseline support needs — for example, significant sensory processing differences, intellectual disability, seizure disorders, genetic syndromes, or regulatory vulnerabilities that affect learning and daily functioning.
Intrinsic complexity reflects the architecture of the nervous system. It shapes developmental pacing and the scaffolding required for learning and stability. But it does not define emotional depth, fulfillment, or potential for growth. It signals conditions that may require sustained support, not fixed limits on what a person can experience or achieve.
Needs also grow at the interface between person and environment. Autistic functioning is highly state‑dependent. Sensory load, predictability, communication clarity, relational safety, and transition frequency all influence how manageable daily demands feel.
In environments that demand rapid social inference, tolerate little processing variability, or remain chronically overstimulating, ordinary autistic differences can escalate into distress, shutdown, or behavioral crisis. What appears to be intrinsic severity may, instead, be prolonged mismatch.
When environmental fit improves (through sensory accommodations, predictable routines, augmentative communication, or pacing adjustments) observed support intensity often decreases. Some forms of complexity, then, are context‑responsive rather than permanent.
A third layer arises from the structure of support systems themselves. Fragmented services, funding instability, eligibility cliffs, staff turnover, and administrative burden can all multiply the coordination work required to sustain care.
Families may spend extraordinary energy navigating systems rather than building skills or stability. Crises may reflect not escalating needs, but inconsistent or inaccessible supports. Here, complexity reflects the fragility of the care environment, not the person alone.
Not all complexity is visible, and that invisibility can be dangerous. Systems most easily recognize need when it is externally disruptive: when classrooms, workplaces, clinics, or families struggle to maintain function. Behavioral escalation, visible dependence, or repeated crises are legible signals — easier to categorize, easier to fund, easier to name “complex.”
Yet many autistic people sustain apparently independent lives through enormous hidden effort. They may speak fluently, achieve academically, hold jobs, or appear socially adept, while relying on intensive invisible supports: unpaid family scaffolding, rigid self‑management, chronic sensory avoidance, exhaustive preparation for interaction, delayed recovery, and sustained energy overuse.
These support loads are not mild; they are merely unobtrusive.
When systems equate visible disruption with real need, they misclassify both groups. Those whose needs interrupt institutional flow are declared “highly complex,” while those who maintain coherence at great personal cost are treated as uncomplicated.
Speech can hide communication vulnerability. Insight can hide regulation difficulty. Professional accomplishment can hide exhaustion. Compliance can hide anxiety. Independence can hide invisible dependence.
This isn’t just mislabeling. It’s delayed risk. Hidden complexity can lead to chronic burnout, health decline, job loss, relational strain, and failure to qualify for assistance until functioning collapses. Many people spend years being told they are “doing fine” while surviving through extreme self‑management.
Recognizing hidden complexity should never minimize the realities of those with visibly intensive support needs. The point is not to collapse difference, but to challenge a model in which only visible struggle counts as complex. A more accurate framework distinguishes between visibility of need and total support load.
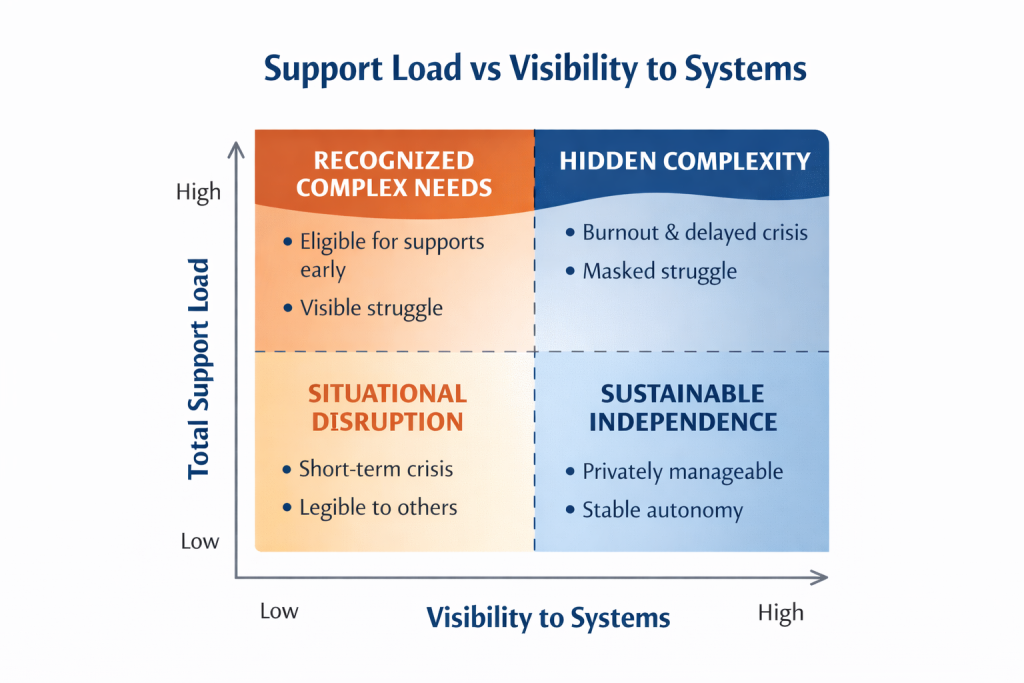
Intrinsic, interactional, and system factors do not simply add together. They multiply. Moderate intrinsic differences can become highly complex when combined with rigid environments or poorly coordinated services. Conversely, even significant intrinsic differences can be sustainably supported when environments are adaptive and systems responsive.
Hidden complexity further complicates this picture. Those whose needs are legible receive structured help earlier, while those whose needs remain concealed may accumulate unsustainable load over time.
Understanding complexity as a systems outcome changes the questions we ask. Not just “How severe are this person’s needs?” but “What conditions are amplifying or reducing the complexity of supporting them?” and “How much human effort is required to maintain the appearance of coping?”
Seeing complexity as co‑created (i.e., among individuals, environments, and systems) reframes policy itself. Instead of ranking people by severity, we could assess the contextual difficulty of sustaining stability: How many adjustments, handoffs, and compensations are required?
Designing services that prioritize flexibility, relational continuity, and environmental fit doesn’t erase intrinsic differences. It prevents them from compounding into crisis.
Complexity isn’t something a person is; it’s something we produce together. And that means we can also design it differently.
"*" indicates required fields